The Ultimate Guide to Wisdom Teeth Removal on the NHS: What You Need to Know
Explore the essential information on wisdom teeth removal NHS. Learn what you need to know for a smooth dental experience.
Introduction to Wisdom Teeth Removal NHS
Wisdom teeth can be a painful and confusing topic for many. These teeth, typically emerging between the ages of 17 and 25, can cause dental problems if not appropriately addressed. Fortunately, the UK's National Health Service (NHS) offers wisdom teeth removal services to qualifying patients. This guide will explore everything you need about wisdom teeth removal NHS, including eligibility, the procedure, recovery tips, and preventative measures.
Understanding Wisdom Teeth
Wisdom teeth, also known as third molars, are the last to emerge in the mouth. They typically appear during late adolescence or early adulthood. While some people may not experience any issues with their wisdom teeth, others may face complications such as:
- Impaction occurs when a wisdom tooth cannot fully emerge because of a lack of space in the jaw or when it grows at an irregular angle, causing it to become trapped beneath the gum line.
- Infection: affected wisdom teeth can lead to infections, which may cause pain, swelling, and difficulty opening the mouth.
- Damage to nearby teeth: affected wisdom teeth can push against the neighbouring second molars, leading to tooth decay, gum disease, or bone loss.
- Cysts: Fluid-filled sacs called cysts can form around affected wisdom teeth, causing damage to the jawbone, nerves, and surrounding teeth.
Eligibility for Wisdom Teeth Removal NHS
The NHS provides dental care for needy patients, including wisdom teeth removal. However, not all cases of wisdom teeth issues qualify for treatment under the NHS. The following conditions may make a patient eligible for wisdom teeth removal on the NHS:
- Severe pain or discomfort caused by impacted wisdom teeth
- Infection or recurrent infections caused by impacted wisdom teeth
- Damage to adjacent teeth, gums, or bone due to impacted wisdom teeth
- Cysts or tumors associated with wisdom teeth
- Difficulty maintaining proper oral hygiene due to the positioning of wisdom teeth
If you believe you may qualify for wisdom teeth removal on the NHS, consult with your dentist. They will assess your situation and determine if you meet the criteria for treatment. Remember, the NHS prioritizes patients with the most pressing dental needs, so we may place you on a waiting list before receiving treatment.
Wisdom Teeth Symptoms
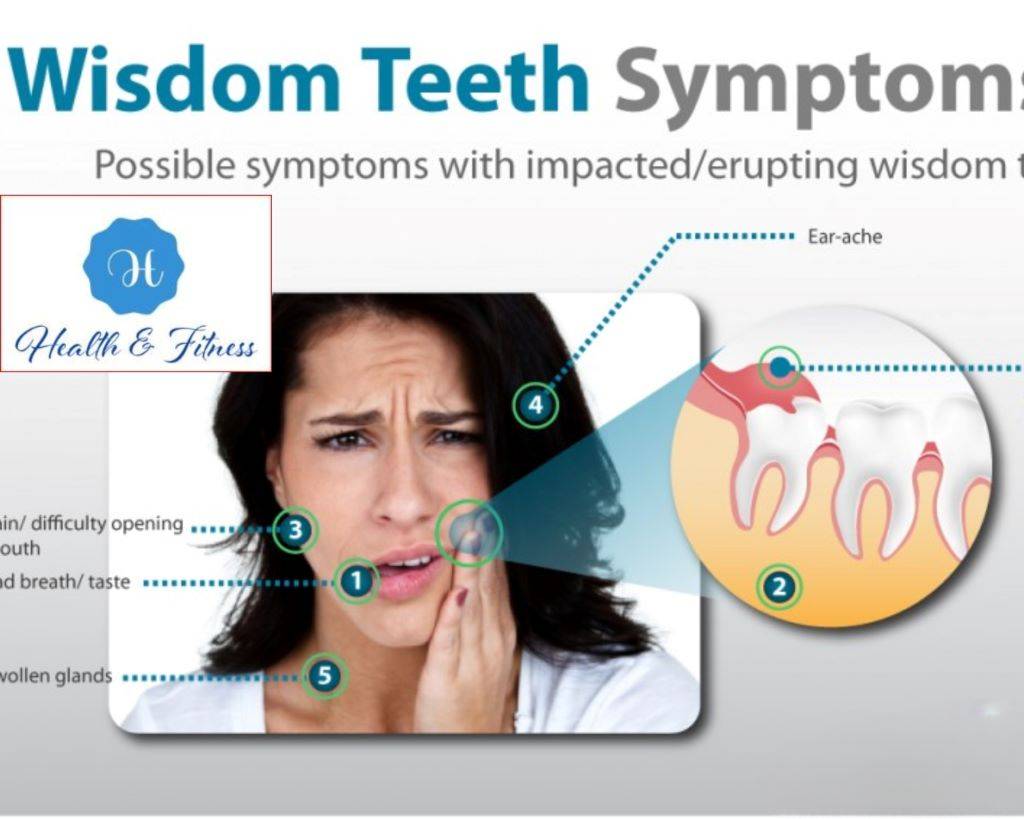
Wisdom teeth, or third molars, can sometimes cause various symptoms when they begin to emerge or become impacted. Here are some common symptoms associated with wisdom teeth issues:
- Pain or discomfort: Pain in the back of the mouth, near the area where the wisdom teeth are located, is a common symptom. This pain can be mild to severe and may worsen when chewing or biting down.
- Swelling and redness: Swelling and redness of the gums around the wisdom teeth can indicate inflammation or infection.
- Breath or unpleasant taste: Impacted or partially erupted wisdom teeth can be challenging to clean, leading to bacterial buildup and resulting in breath or an unpleasant taste in the mouth.
- Difficulty opening the mouth: Pain and swelling around the wisdom teeth can sometimes make it difficult to open the mouth fully or move the jaw comfortably.
- Headaches or jaw pain: Impacted wisdom teeth can cause pressure on the jaw and surrounding nerves, leading to headaches or jaw pain.
- Bleeding gums: Gums around the wisdom teeth may bleed, especially when brushing or flossing.
- Swollen lymph nodes: Sometimes, affected wisdom teeth can cause swollen lymph nodes in the neck or under the jaw.
- Tooth crowding or shifting: As wisdom teeth grow, they can push against neighbouring teeth, causing them to shift or become misaligned.
If you're experiencing any of these symptoms, it's essential to consult with your dentist. They can assess your situation, determine if your wisdom teeth are causing the issues, and recommend appropriate treatment options, such as wisdom teeth removal, if necessary.
The Wisdom Teeth Removal NHS Procedure

Once deemed eligible for wisdom teeth removal on the NHS, your dentist will refer you to an oral surgeon or a dental hospital. The procedure itself will vary depending on the complexity of your case. Generally, wisdom teeth removal can be performed under local anesthesia, sedation, or general anesthesia.
Local Anaesthesia
I can perform most wisdom teeth removals under local anesthesia. The dentist or oral surgeon will numb the area around the wisdom tooth by injecting the local anesthetic. You will remain awake during the procedure but will not feel any pain.
Sedation
If you are anxious about the procedure or the extraction is more complex, the dentist or oral surgeon may recommend sedation. This involves administering a sedative drug, typically through an intravenous (IV) line, to help you relax. You will still be conscious but may not remember much of the procedure afterward.
General Anesthesia
In rare cases, general anesthesia may be required for wisdom teeth removal. This involves administering medication to put you into a deep sleep, ensuring you are entirely unaware of the procedure. Someone typically reserved this for more complicated extractions or patients with specific medical concerns.
The dentist or oral surgeon will create an incision in the gum tissue to expose the tooth and bone during the extraction. They will then remove any bone covering the tooth and may need to divide the tooth into smaller pieces for easier extraction. Once the tooth has been removed, the area will be cleaned, and I will place any necessary sutures to help the gum tissue heal.
Post-Procedure Recovery
Following your wisdom teeth removal, following your dentist or oral surgeon's aftercare instructions is crucial to ensure a smooth and speedy recovery. Here are some general tips for post-procedure care:
- Rest: Resting for the first 24-48 hours after surgery is essential. Avoid strenuous activities as they can increase swelling and bleeding.
- Pain management: Your dentist or oral surgeon may prescribe pain medication or recommend over-the-counter pain relievers such as ibuprofen. Follow their advice on dosage and frequency.
- Ice packs: Apply ice packs to the outside of your face near the extraction site for 20 minutes on and 20 minutes off during the first 24 hours. This can help reduce swelling.
- Diet: Stick to soft, easy-to-chew foods for the first few days. Examples include mashed potatoes, yogurt, applesauce, and smoothies. Avoid hard, crunchy, or spicy foods that may irritate the extraction site.
- Oral hygiene: Gently rinse your mouth with warm saltwater the day after your surgery. Avoid brushing your teeth near the extraction site for the first few days, but continue to brush and floss the rest of your teeth as usual.
- Avoid smoking and alcohol: Smoking can delay healing and increase the risk of complications, while alcohol can interfere with pain medications.
Remember that it is normal to experience some pain, swelling, and bruising after wisdom teeth removal nhs. However, immediately contact your dentist or oral surgeon if you notice any signs of infection, such as fever, severe pain, or pus.
Preventative Measures Wisdom Teeth Removal NHS
While it may not be possible to prevent wisdom teeth from becoming impacted, there are some steps you can take to minimize the risk of complications:
- Regular dental check-ups: Schedule routine dental check-ups and cleanings to monitor the progress of your wisdom teeth and catch any issues early on.
- Early detection: If you are experiencing pain or discomfort related to your wisdom teeth, consult your dentist as soon as possible. Early detection and intervention can help prevent more severe complications.
- Oral hygiene: Maintain a proper oral hygiene routine, including brushing your teeth at least twice daily, flossing daily, and using an antibacterial mouthwash.
Conclusion about Wisdom Teeth Removal NHS
Wisdom teeth removal can be daunting, but understanding the process and what to expect can help alleviate some of the anxiety. If you are experiencing issues with wisdom teeth, consult your dentist to determine if you may be eligible for removal on the NHS. Following the proper aftercare instructions and maintaining oral hygiene can ensure a successful recovery and minimize the risk of complications. Every patient's situation is unique, and this guide is not a substitute for professional dental advice. Always consult with your dentist for personalized guidance on your oral health needs.

Health & wellness writer with 30+ years of experience in nutrition, fitness, and healthy aging. Founder of NextFitLife.com — evidence-based health guidance.



